Congenital anomalies occur for a number of reasons. Approximately every 1 in 33 babies is born with some form of birth
defect, ranging from mild and asymptomatic to life-threatening, and they can be
either preventable (i.e. influenced by the mother and her environment) or
heritable (i.e. genetic). The female reproductive system isn't spared from this possible outcome during fetal development, and there are several types of congenital anomalies that are seen in this biological system.
Birth defects
The differences between birth defects in males and females are most discernible in regards to the external genitalia by which we designate the baby's sex. Female is defined genetically based on the presence of two X chromosomes (genotype 46XX as opposed to male, 46XY), but the absence of male genitalia is considered an indicator of a female at birth. However, abnormal levels of male sex hormones during fetal development due to congenital adrenal hyperplasia, maternal treatment with progesterone, or a maternal hormone-producing tumor can caused alterations to occur in the external female genitalia (e.g., enlarged clitoris). Truly ambiguous external genitalia is referred to as pseudohemaphroditism or virilization. The physical condition is often corrected by surgery after genetic confirmation of sex.
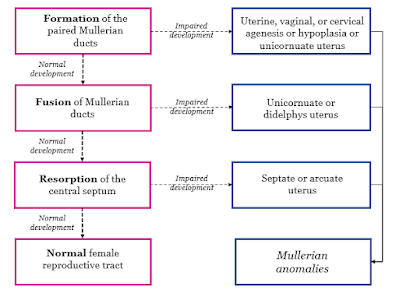 |
| Mullerian duct development. CC By-SA 4.0 Devinka98. Source |
Mullerian anomalies
Defects of the vagina and uterus are called Mullerian anomalies based on their embryonic development from the Mullerian duct. The defects are usually not detected until puberty, when they cause pelvic pain, irregular menstruation, or other reproductive issues, because the ovaries and external genitalia are not affected. The most common defects are agenesis and hypoplasia, in which the tract or part of the tract (such as the vagina) does not form. Whether fertility is affected depends on the exact type and extent of the defect. Some can be surgically remedied to alleviate painful menstruation.
- Unicornuate uterus: only half the uterus forms (banana-shaped). The condition is rare and often accompanied by kidney agenesis.
- Uterus didelphys: double uterus, potentially including duplication of the vagina and cervix.
- Bicornuate uterus: misshaped womb.
- Septate uterus: a wall of tissue divides the uterus.
- Diethylstilbestrol (DES)-related uterus: T-shaped uterus in the child due to maternal exposure to the drug DES; also increases risk of vaginal cancer.
- Arcuate uterus: slight variation in the shape of the uterus, considered simply as a variation of the norm.
Other female reproductive tract defects
- Cloacal abnormalities: The cloaca is the initial tube from which the rectum, urinary tract, and vagina form. Persisting late into development can result in a lack of the appropriate orifices, resulting in severe pain and gastrointestinal disruption, as well as the appearance of male genitalia.
- Imperforate hymen: The vaginal opening is completely blocked, which is discovered when menstruation begins.
- Abnormal ovaries: An extra ovary or extra tissue on the ovaries can occur, as well as ovotestes (presence of both male and female tissues).
Chromosomal abnormalities
When a baby is born with only one sex chromosome it is known as monosomy. X monosomy is referred to as Turner syndrome, or gonadal dysgenesis, and occurs in an estimated 1 of every 2000 live births. Sometimes the second X chromosome is only partially missing. Children born with this condition have swollen hands and feet, and sometimes a wide webbed neck. Puberty doesn't occur and the adolescent lacks secondary sex characteristics unless treated with estrogen. Children may also have a short stature unless treated with growth hormone. Menstruation is absent and an adult with Turner’s is infertile. The condition has a number of complications, including heart defects, autoimmune disorders (e.g., hashimoto’s thyroiditis and diabetes), arthritis, and cataracts.
No comments:
Post a Comment